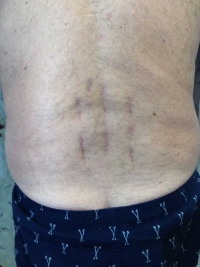
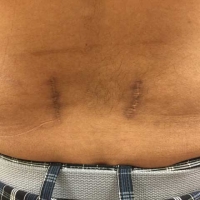
The purpose of a typical decompression spine surgery is to remove any offending compressive structures (bone spur, disc herniation or ligament) that push against the sensitive nerve root. The safest way to mechanically remove the offending structure is under direct visualization. That is-directly observing the nerve while decompressing the structures that cause the compression.
A secondary way to decompress the nerve root is with “indirect decompression”. This normally involves a fusion where the vertebrae are realigned using spacers and/or screws .The realignment should by itself decompress the nerve or canal.
A good surgeon is like a sculptor and opens pathways for the nerve roots by physically removing compressive structures. Any mechanical technique for spine surgery requires “good hands”. The safest way to treat nerves is with small delicate tools to remove adhesions and free the nerve root under direct visualization.
Direct decompression is normally performed under the microscope. The surgeon finds the “plane” between the compressing structure and the nerve root, separates the nerve from the compressive mass with a surgical instrument to protect and retract the nerve safely. The surgeon then removes the compressive mass with another tool such as a bur (like a “Dremel”), a curette (a scraper-like device), a kerrison (a small “biter” device) or an osteotome (a chisel-like device) while the nerve is being protected by the assistant. The assistant looks at the same image as the surgeon through the microscope.
There are structures (ligaments or small veins) that might need to be cauterized near the nerves. These can be safely cauterized with a tool called bipolar cautery. This tool looks like a long thin pair of tweezers. The tips of these tweezers will heat up the area only immediately between the two ends. The surgeon can grasp the problematic structure (normally an adhesion or a small blood vessel) that needs to be cauterized and only this tissue in between the two forceps tips will be impacted with this heat.
The structure that needs to be cauterized can be held away from any nerve and the heat can be produced safely. The heat is only generated between the two tips so that any tissue away from these two tips is not affected. This bipolar cautery method is much more precise than the use of a laser.
Are you a candidate for minimally invasive spine surgery?
Would you like to consult with Dr. Corenman about your condition?
You can set up a long distance consultation to discuss your
current X-rays and/or MRIs for a clinical case review.
(Please keep reading below for more information on this topic.)
Minimally Invasive Spine Surgery (MIS)
To understand why the “minimally invasive” technique and tubes were developed goes back to spine surgery some 30 years ago. Spine surgery was traditionally performed as “open surgery,” meaning the area being operated on is exposed with a long central incision to allow the surgeon to open and access the anatomy. In this old style open surgery, the doctor makes an incision that is 5 to 10 in. long, exposing levels that were not necessary and moves the muscles to each side to see the spine. With the muscles retracted to the side, the surgeon can access the spine to remove bone spurs or herniated disks. The surgeon could also easily see to place screws, cages, and any bone graft materials necessary to fuse the spinal bones and promote healing.
Back in the 1970s, Leon Wiltse in California developed a technique where two separate incisions were made about one inch off the center of the spine, splitting the back muscles to gain access for patients undergoing fusion for spondylolisthesis. This early muscle splitting technique helped to pioneer fusion in these patients who previously had poor fusion success (the TLIF was not yet invented yet by Harms and fusion success at this era was not great).
In response to the very large incisions of the day, the development of the far lateral approach of Wiltse, the poor results of surgery that at the time (with no obvious reasons for failure) and the development of the operating microscope, retractor tubes were invented to create a smaller incision at each level to “reduce tissue trauma”. “Minimally invasive spine surgery” was therefore born to treat spine problems with the thought of less injury to the muscles in the spine. Some other reported advantages of MIS surgery included the report of smaller incisions, less bleeding, and shorter stays in the hospital.
All claims and comparisons of “MIS” surgery however were in comparison to the typical “old style” large open incisions where the surgeons were not concerned about hemostasis (blood loss) or tissue damage.
One of the theoretical drawbacks of large incision open surgery is that the pulling or “retraction” of the muscles can hypothetically damage them. This conjecture has never been proven but is central to the MIS surgeon’s claim that MIS is better. I would agree that the incision length in the original spine surgeries was much too long and probably detrimental to some degree but Minimal Open Spine Surgery incisions are shorter than MIS surgery.
Minimal Open Spine Surgery
At about this same time that MIS surgery was being developed, the O-Arm with Stealth (intraoperative CT scanning with GPS coordinates) was also developed. This machine allowed the surgeon to view a three dimensional reconstruction of the patient’s spine in real time to place the screws and rods necessary for fusion success. This allowed significant reduction of the surgical incision, in many cases to 1½ inches as the anatomy was well visualized without long incisions.
The microscope was also gaining popularity. This device allowed some surgeons to develop the minimal open spine surgery techniques. This was a great refinement of the original surgery that allowed exposure centrally with minimal retraction. This technique allowed great visualization, central access to the canal (important when nerve decompression is necessary) and allows great access to bone graft, so necessary when a fusion is part of the surgical plan.
Since the exposure was limited, so was the blood loss. With these new surgical techniques blood loss is typically the same or less than equivalent MIS surgery.
Problems with MIS Surgery
The idea of MIS surgery using multiple retractor tubes for “minimally invasive” procedures in the lumbar spine has to be evaluated for effectiveness. Does this procedure reduce surgical tissue trauma and make the surgical incision heal more quickly? Is the scar better? Is the technique safer with better results? In my opinion, the answer to all these questions is no. There have been many unsubstantiated claims made about MIS surgery but no head-to-head studies of the two surgeries have been made.
The truth about MIS surgery is that the surgeon’s visibility is less than minimal open spine surgery. This means that surgical decompression of the nerves is less accurate due to less visibility. The MIS technique places the surgeon at the edge of the canal where decompression is more challenging and can create potential injury to neurological structures. The minimal open spine surgery technique places the surgeon directly above the center of the canal. The obvious advantage is with a full and complete decompression if required.
As noted previously, the blood loss is no different in MIS surgery than minimal open spine surgery. The pain is about the same when comparing similar surgeries using the minimally open technique and the recovery time is about the same.
One of the founding premises of MIS surgery is “less tissue damage” and the belief that muscle retraction can cause post-operative pain. These premises are not true if compared to minimal open spine surgery. The incision length is literally twice as long with MIS as with minimal open surgery. The MIS techniques require exposure of both transverse processes. The muscle retraction is about the same in each surgery but the fallacy of MIS surgery preserving muscles is that most MIS surgeons do not perform posterolateral fusions.
Performing a posterolateral fusion in my opinion is critical for success in about 20% of TLIF surgeries. That is, without a posterolateral fusion, I believe that 20% of TLIFs can fail or the fusion can be delayed by 4-6 months.
The muscles that are retracted are all local segmental muscles (they connect from segment to segment) and will be useless after a fusion. To preserve them is pointless when the segments are immovable. If these muscles are preserved, there is a problem with posterolateral fusion. These muscles (multifidi and rotators) occupy the space that the bone graft (and BMP) needs to occupy to create a local one-segment fusion.
The cosmetics of one central incision is superior to the MIS technique with two separate incisions. The single incision spreads less and is more visually appealing.
The last disadvantage of MIS surgery is getting bone graft for the fusion. With a side approach through a tube, this makes getting a bone graft from the removal of the facet difficult.
Good Uses of MIS Surgery
Now there are good reasons to use MIS surgery and tubular retractors. Far lateral disc herniations and posterior cervical foraminotomies are much more effectively treated with these retractors.
During this procedure, an incision is made and the tubular retractor is inserted through the skin and penetrates the muscles down to the spinal column. This creates a tunnel to the region of the surgical disorder. The tubular retractor holds the muscles open and is held in place throughout the procedure by an adjustable arm held in place attaching to the surgical table.
I think that in these circumstances the tube offers a smaller incision and better visualization. You can watch my videos on this website to understand how these techniques work.
If you would like to learn more about the common myths of minimally invasive spine surgery, please contact the office of Dr. Donald Corenman, spine surgeon and back specialist in the Vail, Aspen, Denver and Grand Junction, Colorado area.
Related Content
- Transforaminal Lumbar Interbody Fusion (TLIF)
- Posterolateral Fusion (PLF)
- Anterior Lumbar Interbody Fusion
- XLIF/DLIF Far lateral Interbody Fusion
- Microdiscectomy or Fusion?
- Minimally Invasive Lumbar Fusion
- How to Describe Your History and Symptoms of Lower Back and Leg Pain
- Best Questions to Ask When Interviewing a Spine Surgeon or Neurosurgeon
- When to Have Lower Back Surgery