An Overview of
Transforaminal lumbar interbody fusion (TLIF) is a fusion procedure designed to join one vertebral body to the next. It is used for various problems such as instability, degenerative spondylolysthesis, isthmic spondylolysthesis, discogenic pain, multiple recurrent disc herniations and foramenal collapse.
The TLIF was designed to perform a complete fusion of the front of the vertebra and back of the vertebra (called a 360) through a small incision only in the back of the spine. Before this procedure was developed, there would have to be incisions in the back of the spine and in the belly to achieve this type of fusion success. With the TLIF, the nerves can be decompressed, the disc height reconstructed and the vertebra leveled. If the foramen is collapsed, this method will allow reconstruction of the collapse and freedom to the crushed nerve.
Are you a candidate for Transforaminal Lumbar Interbody Fusion (TLIF)?
Would you like to consult with Dr. Corenman about your condition?
You can set up a long distance consultation to discuss your
current X-rays and/or MRIs for a clinical case review.
(Please keep reading below for more information on this treatment.)
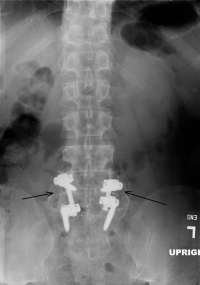
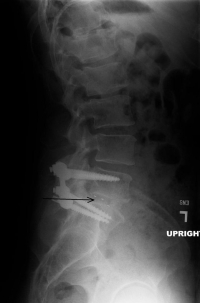
It is performed just as it sounds (unlike 99% of descriptions in medicine). The surgery is done through the foramen (transforaminal) in the lumbar spine into the disc space in between the two vertebral bodies (interbody) to create a fusion. An incision is made midline on the spine (normally about 2 ½ inches long). The two vertebrae are exposed and the transverse processes are exposed on the sides of the vertebra. 4 pedicle screws are place into the vertebrae. The vertebra are the distracted through tools that push the screws apart. The microscope is brought into the field.
The facet from the superior and inferior vertebra on one side are removed. These facets are cleaned, ground up and reused as bone graft. For this procedure, we never have to take bone from the pelvis anymore.
One bonus is that taking the facets on one side solves any type of preexisting foramenal stenosis as the facets themselves cause this condition and are removed.
The disc is opened and any debris remaining in the disc is removed. Remember that this procedure is performed for patients with degenerated discs and a normal disc is never seen as there would be no reason for a in the first place. The disc is spread apart with an interdiscal spreader (a mechanical tool to restore the disc height).
Three things are placed in the disc to hold it apart and get it to fuse together. The first is BMP or bone morphogenic protein. This is a synthetic human protein that causes your own stem cells to turn into bone cells. The second is the ground up facet bone previously removed and cleaned. The last is a little plastic cage that holds the vertebra apart. This is essentially a spacer to hold the vertebra distracted while the bone heals.
The incision is irrigated copiously to wash out any aberrant BMP (you would not want bone to form in the canal) and a Valsalva maneuver is performed to make sure there is no dural leak.
At this point, if there is any further canal decompression to perform, it is done now with the microscope still in the field.
The microscope is removed and the distraction of the screws is taken down. Some bone and BMP that was not placed in the disc space is now placed along the sides of the vertebra on the remaining lamina, facets and transverse processes. Rods are then connected to the screws and tightened down and a small amount of morphine is placed in the spinal canal to control pain overnight.
During the entire transforaminal lumbar interbody fusion (TLIF) procedure, the patient is monitored electronically to make sure the nerves and spinal cord are functioning properly. Any blood loss is recycled through a device called a cell saver. The blood is washed and given back during the actual procedure to minimize blood loss. (All Jehovah’s Witnesses have the procedure performed without cell saver).
The incision is closed and the patient is discharged to the recovery room.
For additional information on
Related Videos
Related Content
- Posterolateral Fusion (PLF)
- Anterior Lumbar Interbody Fusion
- XLIF/DLIF Far lateral Interbody Fusion
- Microdiscectomy or Fusion?
- Minimally Invasive Lumbar Fusion
- Myths of Minimally Invasive Spine Surgery
- Myths of Laser Spine Surgery
- Indications for Lumbar Fusion
- X-Stop Procedure
- Artificial Disc Replacement (ADR) for Lumbar Spine