Overview
is a fusion in the front of the spine from an approach through the abdominal wall and the belly.
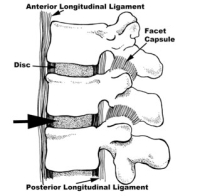
The fusion occurs in between the vertebral bodies. The procedure starts with removal of the anterior annulus and anterior longitudinal ligament (ALL) which both sit in the front of the spine. The remnants of the nucleus are then removed, the bony endplates are cleared of cartilage down to cortical bone and a spacer is placed with bone graft material.
The spacer can be made of allograft (donor bone), the patient’s own bone (normally from the iliac crest) or from a material like PEEK (plastic or polyether ether ketone) or titanium. This spacer can be held in place with additional screws if the surgeon chooses.
The fusion material in the spacer can be made of donor bone, the patient’s own bone, a bone “substitute” or BMP (bone morphogenic protein).
The advantage of the ALIF is that the entire disc can be visualized when cleared. This is valuable especially when there was a previous attempt at fusion that was unsuccessful (a pseudoarthrosis), particularly a TLIF failure. The anterior approach is also valuable when there is a large slip of a vertebra such as in the case of a grade III isthmic spondylolisthesis (more than half of the vertebra is slipped off the sacrum-see website).
If there is a great need to restore alignment, the anterior approach has some advantages. The anterior disc wall and the anterior longitudinal ligament are removed which allows greater distraction of the anterior portion of the disc space. This creates more back angulation (lordosis) and if necessary, can restore the sagittal (side view) alignment of the spine.
Generally, if an is performed, many surgeons will “back this procedure up” with posterior instrumentation (pedicle screws and rods) in the rear of the spine. This of course, requires a separate incision in the rear of the spine.
Are you a candidate for Anterior Lumbar Interbody Fusion (ALIF)?
Would you like to consult with Dr. Corenman about your condition?
You can set up a long distance consultation to discuss your
current X-rays and/or MRIs for a clinical case review.
(Please keep reading below for more information on this treatment.)
There are some greater risks with the anterior approach compared to the posterior approach that needs to be considered if an ALIF is planned. The anterior abdominal wall muscles have to be incised. This can create a weakness of the wall and an out pouching (diastasis) that looks like a hernia.
It the patient is rotund or thick, the approach is more difficult as the depth to the spine will be greater.
The great vessels need to be mobilized. This can be tricky especially at L5-S1 if the bifurcation (splitting) of the vena cava into the common iliac veins is very low.
In males, there is a fine network of nerves called the sympathetic plexus that needs to be moved, especially at the lowest lumbar level. If these nerves become non-functional (1-5% of the time), the male can experience retrograde ejaculation. That is, the ejaculate will occur but will travel into the bladder instead of exiting out the end of the penis.
Both male and female may experience one warm leg compared to the other after surgery. This occurs when the same sympathetic nerve complex becomes damaged. These nerves regulate blood flow to the legs and damage to one side will allow blood to flow unregulated to that leg. Hence- that leg will feel warmer.
Also, the procedure causes scar to occur. Any return visit to this surgical site is fraught with difficulty as the great vessels can scar down. It is uncommon but not unheard of to have some bowel adhesions too.
For additional resources on
Related Content
- XLIF/DLIF Far lateral Interbody Fusion
- Microdiscectomy or Fusion?
- Minimally Invasive Lumbar Fusion
- Myths of Minimally Invasive Spine Surgery
- Myths of Laser Spine Surgery
- Indications for Lumbar Fusion
- X-Stop Procedure
- Artificial Disc Replacement (ADR) for Lumbar Spine
- Transforaminal Lumbar Interbody Fusion (TLIF)
- Posterolateral Fusion (PLF)