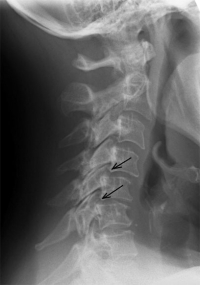
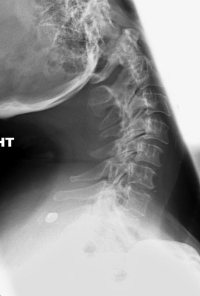
Overview of Cervical Spine Instability
Painful excessive motion of the vertebral bodies within the cervical spine in relation to one another is considered cervical spine instability. Instability in this region will make a patient feel as if the neck and upper spine are moving at a greater movement than what the bone, muscle and ligament can hold. The feeling is that a patient must be careful with head motion or a sharp pain and “catch” will occur. The motion must be reproducible with the same motion at most times to be considered instability. That is, if it occurs only one a week, it would not be considered unstable but if it occurs 5-8 times a day, instability would be considered as a diagnosis. This dysfunction of the spinal cord often leads to other issues of the spine leading to a disruption of normal everyday activities.
The cause of cervical spine instability is normally the result of the natural wear and tear degenerative changes of the cervical spine or arthritis of the neck, as well as a previous injury or congenital condition. Patients with a herniated disc (some refer to it as a slipped disc but this is often another condition) may suffer from instability. The entire motion unit (both disc and facet) must wear in a manner that the normal restraining structures become deficient. The resultant instability causes the patient to forego activities that would put their neck at risk.
Symptoms of Cervical Spine Instability
Symptoms of cervical spine instability include sharp neck pain with motion or position, upper back pain, and an acute, on-going unstable sensation within the region. Muscle spasms of the neck and spasms in the back are also a common occurrence for patients experiencing instability as the muscles work overtime to try and prevent the painful motion.
Are you suffering from symptoms of cervical spine instability?
Would you like to consult with Dr. Corenman about your condition?
You can set up a long distance consultation to discuss your
current X-rays and/or MRIs for a clinical case review.
(Please keep reading below for more information on this condition.)
Treatment of Cervical Spine Instability
Non-Surgical
Non-surgical treatments are typically enough to restrain the symptoms of cervical spine instability and many injuries of the spine including patients with spasms in the back. Non-steroidal, anti-inflammatory medication along with physical therapy and prescribed exercises typically work well. Ergonomics are important to prevent putting the neck in a position of instability (typically a flexion and twisting motion). Adjusting the stem height on a bicycle seat and adjusting the golf swing are good examples. Chiropractic manipulation is not recommended as these segments move too much and manipulation would increase the motion.
Surgical
If these non-surgical remedies do not work, and the patient is having ongoing spasms in the back and instability, then surgery for neck instability involving stabilization and fusion will most likely be the next course of treatment. The anterior cervical decompression and fusion (ACDF) procedure is performed for cervical spine instability, painful degenerative disc disease, bone spur, compressed nerve (neck), or spinal cord, herniated disc, or even a fracture of the cervical spine.
For more information on cervical spine instability, please contact Dr. Donald Corenman, spine specialist and neck doctor serving the Vail, Aspen, Denver and Grand Junction, Colorado communities.
Related Content
- Cervical Radiculopathy or Pinched Nerve in the Neck
- Cervical Herniated Disc
- Arthritis of the Neck and Back
- Cervical Deformity
- Cervical Degenerative Kyphosis
- Cervical Degenerative Spondylolisthesis
- Cervical Central Stenosis & Myelopathy
- Chronic Radiculopathy
- Cervical Degenerative Disc Disease
- Cervical Degenerative Facet Disease
- How to Describe Your History and Symptoms of Neck, Shoulder and Arm Pain
- Best Questions to Ask When Interviewing a Spine Surgeon or Neurosurgeon
- When to Have Neck Surgery
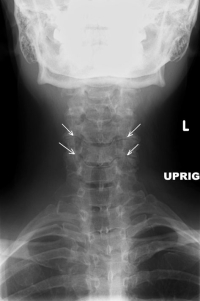
(Click to Enlarge Image) AP X-ray of severe degenerative facet disease that leads to instability. The white arrows point to the worn facets.