Cervical Degenerative Facet Disease Overview
The cervical facets differ from the lumbar facets in many ways. First, the lumbar facets carry less than 10% of the entire weight of the lower back but the cervical facets, because of their larger size; carry over 30% of the cervical spine weight. The facet’s larger surface area and greater weight carrying capacity cause these facets to be subjected to greater forces. These forces can cause destructive wear and tear and result in typical arthritis.
Anatomy
The facets are a true diarthrodial joints. This means the facet is really a classic joint that we think of like a knee, hip or shoulder joint. This joint complex consists of two smooth bony surfaces each covered with a very slippery coating called hyaline cartilage where they touch. The joint itself is held together with a tough fibrous outer sack called the capsule. The capsule literally pulls the joint surfaces together and prevents extreme motion by acting like a checkrein ligament. The inside of the capsule is lined with a slim layer of cells called the synovium. These cells produce a very thin, slippery liquid called synovial fluid, which lubricates these joints.
If a pressure transducer probe is inserted into any diarthrodial joint, you would find that the joint itself is under negative pressure or suction. This negative pressure is one of the protective forces that hold the joint together. This is not dissimilar to the suction that holds the bottom of a wet glass onto a glass coffee table. Removing the glass takes some force to break the vacuum between the table and the glass. When the glass finally releases, a slight “pop” is heard when the suction bond is broken. This is the same pop that is produced with a chiropractic adjustment.
Abnormal wear of the cartilaginous surfaces can occur under many circumstances. Degenerative disc disease can cause abnormal motion to the facets. Injury to the ligaments that hold the joint together (including the capsule) causes abnormal wear. Simple genetics can cause wear of the facets. This wear destroys the suction bond that holds the joint together.
Facet Function
Mechanically, the intact facet has three purposes. The first purpose is to guide the spine in specific directions of motion. Facets, depending upon how they are anatomically angled, allow flexion/extension, lateral bending and rotation. These joints also demonstrate coupled motions. That is, strict lateral bending will also cause rotation of the vertebra.
The second purpose of the facet is to bear weight. Approximately 30% of the weight of the head is transmitted into the shoulders through the facets (the other 70% is transmitted through the discs). The amount of weight bearing percentage changes with bending the head forwards vs. backwards and side to side. Backwards bending (extension) produces increased load and therefore pressure to be placed on the facets. Patients with facet pain normally will have increased neck pain with this motion.
The last function of the bilateral facets is that of a doorstop. The upper facets are angled backwards and “hook into” the lower facets of the vertebra below. This link prevents the upper vertebra from sliding forward on the lower vertebra (I like to call this the doorstop mechanism). When the facets wear out, this link is broken and the upper vertebra can abnormally slide forward on the lower vertebra (degenerative spondylolisthesis or anterolisthesis). This shifting can be painless or produce instability pain along with possible nerve and spinal cord impingement.
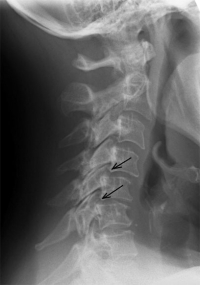
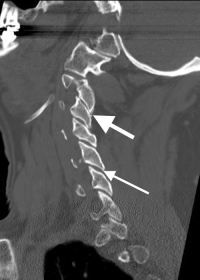
(Click to Enlarge Image) Lateral X-Ray of the neck with a forward bend (flexion). Note the vertebra slipping forward. The black arrows point to the forward slide and forward angulation of the vertebra.
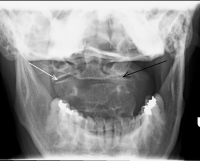
(Click to Enlarge Image) This patient developed unilateral (one-sided) arthritis of the facet of C1-2. Black arrow points to the arthritic facet and the white arrow points to the normal facet. She has pain with rotation of the head and rotation is limited. This X-ray is called an open mouth odontoid as it is taken through an open mouth to visualize the C1-2 facet joints.
Are you suffering from symptoms of cervical degenerative facet disease?
Would you like to consult with Dr. Corenman about your condition?
You can set up a long distance consultation to discuss your
current X-rays and/or MRIs for a clinical case review.
(Please keep reading below for more information on this condition.)
Symptoms of Cervical Degenerative Facet Disease
Facet degeneration or arthrosis causes four potential symptoms; neck pain, headaches, arm pain from foraminal stenosis (compression of the nerve root) and instability pain (degenerative spondylolysthesis with potential spinal cord compression).
Local neck pain is probably the most common symptom of facet pain. When the cartilaginous surfaces wear off and bone to bone contact is the result, deep dull local bone ache is common. Sharp pain with movement occurs when neck motion overloads these surfaces. Stiffness and joint noises (clicking and popping) typically occur. This pain can radiate into the shoulders.
The upper cervical joints (C2-3 and C3-4) can cause headaches along with local pain due to their proximity to two particular nerves; the greater occipital nerve-C2 and the lesser occipital nerve- C3 (AKA greater auricular nerve). The greater occipital nerve originates from C2 and radiates up over the skull to end at the forehead. The lesser occipital nerve originates from C3 and radiates around the ear to the temple. These two nerves can cause suboccipital headaches (headaches that originate from the base of the skull and radiate to their respective terminus). Interestingly, the C2-3 and C3-4 facets do not have to have significant degenerative appearances on MRI or CT scan to cause this type of pain.
Facets develop bone spurs when they become arthritic. These bone spurs can grow into the foramen and compress the spinal nerve (pinched nerves). This in turn will cause pain that radiates down the distribution of the nerve. Each nerve has a specific route of pain that will be produced. If the C3 nerve is involved, pain will radiate from the base of the skull around the ear and terminate at the temple. If the C7 nerve is involved, pain will radiate from the shoulder into the middle of the hand. This condition is covered more thoroughly in the foraminal stenosis section on this website.
Many times, arthritic facets will not be painful even with advanced arthritis. However, the wear of the facets will allow some increased play in the “doorstop mechanism”. This sloppiness can allow a forward slip of one vertebra on the other and will increase the strain on the disc. This, in turn can lead to annular tears of the disc, which then starts the degenerative cascade of degenerative disc disease. In addition, the wear of the facets can allow a forward slip of the vertebra above on the vertebra below leading to a degenerative spondylolisthesis. This shifting can cause local neck instability pain or can cause intermittent compression of the nerve roots or even spinal cord compression.
Treatment of Cervical Degenerative Facet Disease
Treatment of facet disease depends upon the symptoms, the biomechanics and the source of pain. There are many individuals that have facet disease without pain. The reason for the lack of pain in some individuals while others have incapacitating pain is a Nobel Prize winning answer.
Simple facet pain responds to many therapies including chiropractic, physical therapy, massage and even acupuncture. For more advanced pain that fails these treatments, injection therapy in the form of facet blocks or medial branch blocks (see website under injections for more information) can be effective.
Rhizolysis (the burning of the small sensory nerves that innervate the joint through a small needle) can be very effective in the right hands under the right circumstances.
Finally, surgery can be very effective. If a pinched nerve develops from facet arthritis, a posterior foraminotomy can be effective (as long as there is also no anterior bone spur off the uncovertebral joint). For instability from a degenerative spondylolisthesis or from severe pain due to a very arthritic facet, fusion is required. Artificial discs will not work in this circumstance.
To discuss cervical degenerative facet disease in more detail, please contact the office of Dr. Donald Corenman, spine specialist and neck doctor offering diagnostic and surgical second opinions to patients in the USA and around the world.
Related Content
- How to Describe Your History and Symptoms of Neck, Shoulder and Arm Pain
- Best Questions to Ask When Interviewing a Spine Surgeon or Neurosurgeon
- When to Have Neck Surgery
- Cervical Herniated Disc
- Arthritis of the Neck and Back
- Cervical Deformity
- Cervical Degenerative Kyphosis
- Cervical Degenerative Spondylolisthesis
- Cervical Central Stenosis & Myelopathy
- Chronic Radiculopathy
- Cervical Degenerative Disc Disease
- Cervical Spine Instability