An Overview of Far Lateral Disc Herniations
of the Lumbar Spine
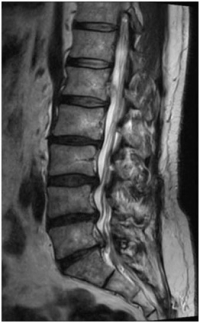
“Normal” disc herniations in the lumbar spine occur in the posterolateral position. This is a spot in the spinal canal where the traversing nerve lies. About 95% of the time when a disc herniation occurs, the herniation will occur in this posterolateral position and compress the nerve in the canal.
The reason for the herniation being so common in this location is that the walls of the disc are thinnest and therefore weakest here. This is the site that normally tears through and through. The jelly (nucleus) of the disc will push out (herniate) and compress this traversing nerve. The symptoms are typically pain in the buttocks and leg with sitting that are relieved with standing. There are of course, some exceptions to this rule. See the section on lumbar disc herniations to better understand this concept.
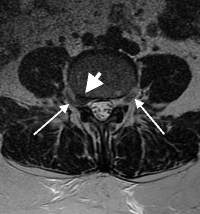
2-5% of the time, a disc herniation in the lumbar spine will occur in the far lateral position. This location is part of the spine outside the spinal canal. The exiting nerve travels through the foramen (exit hole) and lies next to the disc wall here. A far lateral disc herniation will compress the nerve. The nerve becomes tented over the herniation as it exits into the muscle (the psoas) on the side of the spine. Symptoms include buttocks and leg pain but unlike the typical posterolateral herniation, this far lateral herniation can cause pain that may be increased with standing.
Depending upon the nerve involved, pain may occur in the back of the thigh or the front of the thigh and may radiate all the way down the leg. Pain, paresthesias (pins and needles) and numbness are the typical symptoms that may occur with a far lateral disc herniation.
Depending upon the nerve that is affected, weakness may be noticed in the foot (foot drop) or the thigh (quadriceps weakness). If the weakness occurs in the foot, the foot may slap on the ground when walking. Patients with foot drop may trip over their own foot when taking a step. With quadriceps weakness, climbing stairs, getting out of a car or stepping up onto a curb may feel “spongy” or the knee will feel like it will want to “give out”. Falls can occur with quick motions.
Even a radiologist may miss a far lateral disc herniation as the MRI findings may be subtle. The radiologist unfortunately does not have the clinical suspicions developed from actually examining a patient and be unaware of the process causing pain or weakness in a specific nerve.
Are you suffering from symptoms of a far lateral disc herniation?
Would you like to consult with Dr. Corenman about your condition?
You can set up a long distance consultation to discuss your
current X-rays and/or MRIs for a clinical case review.
(Please keep reading below for more information on this condition.)
Treatment of a Far Lateral Disc Herniation
Treatment of this lumbar spine disorder is based upon the standard protocol for any disc herniation and is covered by the section on this website under “When to have lumbar surgery”. Many times, surgery can be avoided with proper care. If weakness of a muscle group is noted, unfortunately this is an important indication to consider surgery.
When surgery is required, the surgery is different than the typical posterolateral microdiscectomy. The far lateral herniation is approached through an incision about 3 cm off of midline and splits the erector spinae muscle (the muscle that causes the spine to bend backwards). Since the fibers of the muscle run in line with the incision, this approach is not significantly traumatic.
During the far lateral microdiscectomy, the spinal canal is not entered and the fragment is removed from the side of the spine. Click on the video of the actual surgery to the right if you have unanswered questions.
For additional resources on a far lateral disc herniation of the lumbar spine, please contact the practice of Dr. Donald Corenman, spine specialist and back doctor offering diagnostic and surgical second opinions to patients in the USA and around the world.
Related Content
- When to Have Lower Back Surgery
- Causes of Lower Back Pain
- Normal Spinal Alignment
- Lumbar Spine Anatomy
- How to Describe Your History and Symptoms of Lower Back and Leg Pain
- Best Questions to Ask When Interviewing a Spine Surgeon or Neurosurgeon
- Degenerative Spondylolisthesis
- Isolated Disc Resorption-Lumbar Spine (IDR)
- Lumbar Spinal Stenosis (Central Stenosis)