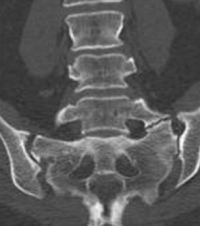
Overview
The sacrum is made of five separate pieces of bone that fuse to each other in utero (when we are developing at the fetus stage in the uterus). While these sacral segments are fusing, confusion can happen. The L5 vertebra can take on characteristics of the sacrum. The transverse process of L5 can enlarge and develop an articulation to the sacrum (see image). This abnormal joint is called a transverse-alar articulation or a sacralization of L5.
Normally when this unusual malformation occurs, the transverse-alar articulation stabilizes this level and the vertebra does not move. This protects and prevents loading of the L5-S1 disc, which prevents degeneration and pain.
There is however, a smaller subset of patients that has this sacralization syndrome with pain. In these patients, this articulation does move slightly enough to cause pain. This is the cause of Bertolotti’s Syndrome.
is very uncommon. Many patients diagnosed with this disorder are more likely instead to have a degenerative facet or nerve root irritation in the lower lumbar spine. This can be proven with the appropriate diagnostic block (see website under lumbar degenerative facet or lumbar radiculopathy).
Are you suffering from symptoms of Bertolotti’s Syndrome?
Would you like to consult with Dr. Corenman about your condition?
You can set up a long distance consultation to discuss your
current X-rays and/or MRIs for a clinical case review.
(Please keep reading below for more information on this condition.)
Diagnosis and Treatment of
Patients with Bertolotti’s Syndrome typically have lower low back pain only on one side (unilaterally). This disorder is first suspected by standard X-rays where the malformation is identified. Then, an MRI is performed to look at this articulation. If there is the presence of degenerative changes within the bone, the diagnosis is entertained.
Confirmation of Bertolotti’s Syndrome is demonstrated with an anesthetic block right into the transverse-alar articulation and good temporary relief noted (see pain diary).
Treatment starts conservatively. The diagnostic injection not only contains an anesthetic agent but in addition, a steroid. The steroid has the capability of reducing inflammation and possibly yielding long-term relief. If no relief is noted, the next step is an ablation or rhizotomy of the small nerves that surround this joint. This procedure is performed on an outpatient basis using a small needle with a tip that heats up to cauterize these small nerves.
If that ablation/rhizotomy treatment is ineffective, the last step is surgery. The transverse-alar joint can be fused or removed. Removal is slightly simpler surgery but has less of a success rate. Fusion results in no real loss of any range of motion and has a higher success rate but takes longer to recover than the joint removal.
For additional resources on , please contact the office of Dr. Donald Corenman, spine specialist and back doctor offering diagnostic and surgical second opinions to patients in the USA and around the world.